Vitamin D Deficiency Linked To Higher Risk of Early Onset Dementia
New research identifies 15 factors tied to increased risk of early-onset dementia.
By: George Citroner | The Epoch Times
Forgetfulness and confusion, once considered normal signs of aging, are now increasingly striking adults at the peak of their careers. Rates of early-onset dementia and Alzheimer’s disease among Americans younger than 65 have inexplicably doubled between 2013 and 2017, according to data from Blue Cross Blue Shield, a health insurance provider.
Now, new research identifies vitamin D deficiency, which affects 35% of adults in the United States, among 15 adjustable lifestyle factors that appear to drive up a person’s early dementia risk. While the findings also highlight alcohol abuse and isolation, the surprising link between low vitamin D levels and early cognitive decline suggests a simple daily supplement may help the fight against this baffling rise.
Largest Study of Its Kind
The average age of someone between 30 and 64 years old living with either young-onset dementia or Alzheimer’s is 49, with women being disproportionately affected compared to men, according to the BCBS data.
In a recent large-scale study published in JAMA Neurology, researchers identified 15 lifestyle and health risk factors associated with early-onset dementia. The study analyzed information from over 356,000 people younger than 65 whose data were in the UK Biobank, a large-scale biomedical database and research initiative in the United Kingdom, between 2006 and 2010.
“This is the largest and most robust study of its kind ever conducted,” David Llewellyn of the University of Exeter said in a press statement. It is also the first to suggest people can take actions to reduce their risk of the condition by targeting an array of different factors, he added.
Risk Factors for Young-Onset Dementia
“Young-onset dementia has a very serious impact, because the people affected usually still have a job, children, and a busy life,” Stevie Hendriks from the Department of Psychiatry and Neuropsychology at Maastricht University in the Netherlands and lead author of the study said in the statement. “The cause is often assumed to be genetic, but for many people we don’t actually know exactly what the cause is.”
Major contributing risk factors included alcohol abuse, stroke, and hearing impairment—all previously identified as risks for cognitive decline.
However, the study also identified some additional risk factors associated with early-onset dementia that have not been previously explored in depth, including vitamin D deficiency, high levels of inflammatory C-reactive proteins, specifically in women, orthostatic hypotension (low blood pressure that happens when standing after sitting), and social isolation.
Vitamin D Reduced Dementia Risk by 40%
Previous epidemiological studies have also linked vitamin D deficiency with an increased risk of dementia, Claire Sexton, senior director of scientific programs and outreach at the Alzheimer’s Association, told The Epoch Times.
However, relatively few studies have specifically examined risk factors for young-onset dementia, making Ms. Hendriks and team’s study “a welcome addition to the literature,” Ms. Sexton said.
One relevant study, published in the Alzheimer’s Association’s journal Alzheimer’s & Dementia: Diagnosis, Assessment & Disease Monitoring, compared dementia onset between people who took vitamin D supplements versus those who did not. The study included 12,388 Americans without a dementia diagnosis at baseline, with an average age of 71.
The study found that among those who developed dementia within 10 years, about 75% were non-supplement takers compared to only 25% who took vitamin D supplements. Supplementation provided greater protection for women, though it reduced dementia risk in both sexes.
Interestingly, the study found vitamin D seemed to offer more benefit if people supplemented it before there were signs of cognitive problems. “Vitamin D effects were significantly greater in females versus males and in normal cognition versus mild cognitive impairment,” the authors wrote.
Overall, the researchers associated vitamin D supplementation with a 40% lower incidence of dementia compared to no supplementation.
“However, the results of randomized controlled clinical trials of vitamin D interventions on cognitive performance have been mixed,” Ms. Sexton said, noting that further research is needed to confirm the link between vitamin D deficiency and dementia risk.
The Risk Factors We Can Change
Of the risk factors identified in the recent study, several stand out as addressable through lifestyle changes. These include alcohol abuse, diabetes, heart disease, and stroke—with the latter two being linked to high blood pressure, itself a dementia risk factor.
With the exception of Type 1 diabetes, moderate exercise, smoking cessation, and dietary improvements can mitigate these.
More difficult to tackle is loneliness, termed “social isolation” by the researchers. Participants visiting friends and family less than monthly showed higher young-onset dementia association compared to more frequent visitors.
According to U.S. Surgeon General Vivek Murthy, even before the COVID-19 pandemic, about half of American adults reported experiencing loneliness. He recommends taking steps to reduce feelings of social isolation, like answering a phone call from a friend, making time to share a meal, and listening to someone without looking at your cellphone.
“Social isolation is linked to depression, but depression did not mediate the association of social isolation with YOD (young-onset dementia) in our analyses, suggesting that both directly contribute to dementia risk,” the study authors wrote.
To help prevent early-onset dementia, experts recommend making lifestyle changes to mitigate key risk factors like vitamin D deficiency, inflammation, low blood pressure, and social isolation. The following are some tips:
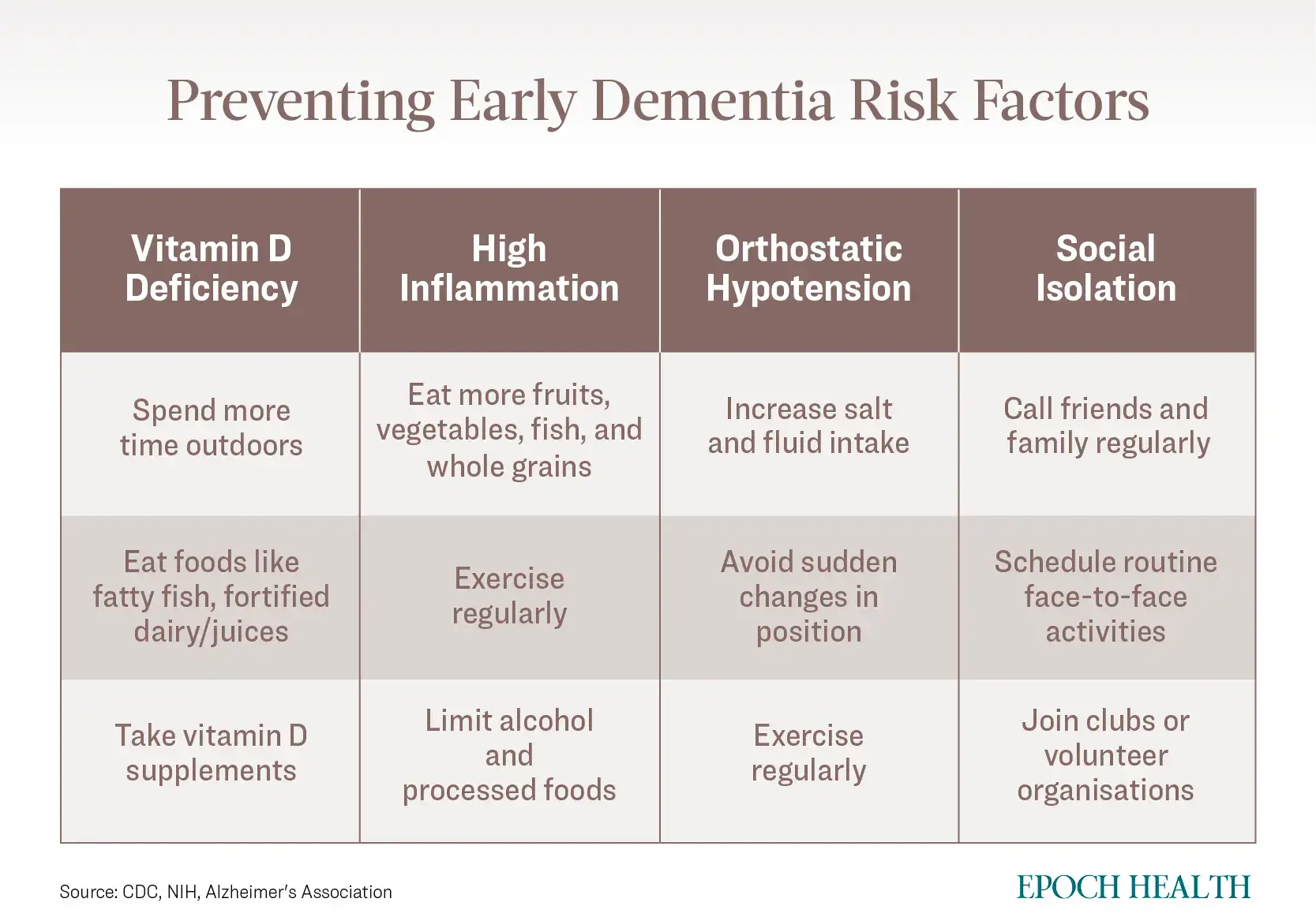
* * *
Must Have: Boost your vitality and support overall wellness with our potent vitamin supplement, providing essential nutrients for a healthier and more energized you.
* * *
NEXT UP!
Can A Dental Infection Cause A Massive Heart Attack?
For literally hundreds of years now, the idea that a dental infection could seed, initiate, and promote virtually all chronic degenerative diseases has been hotly debated in the medical and dental communities, often with much more passion and hyperbole than with science.
This “debate” continues today, and nothing encapsulates this focal infection link between the mouth and the body better than the root canal-treated tooth. And while the root canal-treated tooth is certainly not the only significant source of dental infection and toxicity, it is easily the most devastating one—as you will soon see.
Conventional Dentistry Refuses to Inform Patients about the Risk of a Dental Infection from a Root Canal Procedure
The “success” of a root canal-treated tooth for a given individual depends on the goal of the root canal procedure. If the goal of a root canal procedure is to retain a pain-free natural tooth for both esthetic and chewing function, then the root canal procedure is frequently “successful.”
* * *
READ MORE: Brisk Walking May Help Cut Diabetes Risk by Nearly 40%
Awareness! 7 Reasons To Abandon Your Comfort Zone & Why You’ll Never Regret It
Telegram: Stay connected and get the latest updates by following us on Telegram!
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Collective Spark Story please let us know below in the comment section.
