
Scientists May Have Discovered Why COVID Hits Fat People Harder
Since the beginning of the pandemic, one of the most common denominators in deaths and severe COVID is obesity.
By Tyler Durden | Zero Hedge
Since the beginning of the pandemic, one of the most common denominators in deaths and severe COVID is obesity.
Pre-vaccine, 73% of those who died of (or with) Covid-19 were either overweight or obese – which tracks with the percentage of overweight and obese Americans.
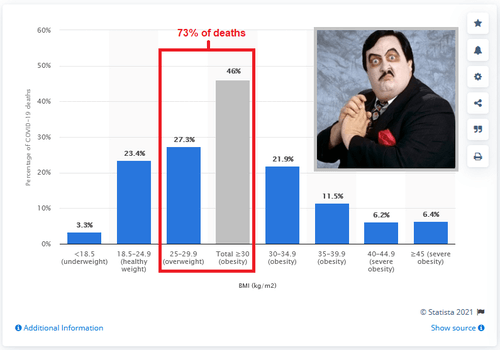
In addition to having generally poor circulatory health, an obese person is more likely to have other conditions that are risk factors for severe COVID, including low-level inflammation, diabetes and lung disease.
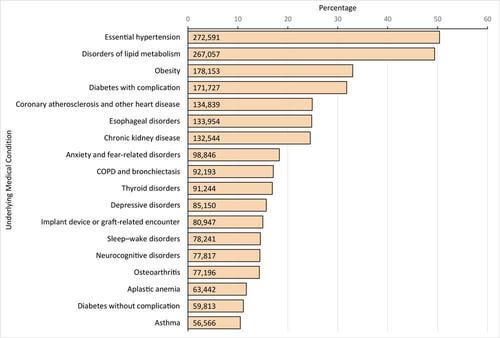
A September 2020 meta-analysis suggested a linear relationship between BMI and Covid-19 severity and mortality.
Meanwhile, and this is unrelated to the point of this article – 75% of COVID deaths to date (unvaxxed and vaxxed) in the United States are retirement age or older, with another 18% between the ages of 50 and 64-years-old. So the vast majority of US COVID deaths are in older Americans, 73% or so of whom are overweight or obese.
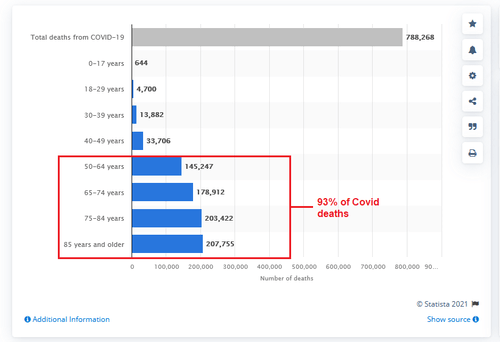
Number of coronavirus disease 2019 (COVID-19) deaths in the U.S. as of December 8, 2021, by age*
Now, scientists may have a clue as to why COVID affects fat people more severely – it infects both fat cells and certain immune cells within body fat, prompting the body to respond aggressively, according to the New York Times, citing a study published in October.
“The bottom line is, ‘Oh my god, indeed, the virus can infect fat cells directly,'” said Dr. Philipp Scherer, a scientist who studies fat cells at UT Southwestern Medical Centre in Dallas, who was not involved in the research.
“Whatever happens in fat doesn’t stay in fat,” he continued. “It affects neighbouring tissues as well.”
The research has not yet been peer-reviewed or published in a scientific journal, but it was posted online in October. If the findings hold up, they may shed light not just on why patients with excess pounds are vulnerable to the virus, but also on why certain younger adults with no other risks become so ill.
The study’s senior authors, Dr. Tracey McLaughlin and Dr. Catherine Blish of the Stanford University School of Medicine, suggested the evidence could point to new COVID treatments that target body fat.
* * *
The finding is particularly relevant to the United States, which has one of the highest rates of obesity in the world. Most American adults are overweight, and 42% have obesity. Black, Hispanic, Native American and Alaska Native people in the U.S. have higher obesity rates than white adults and Asian Americans; they have also been disproportionately affected by the pandemic, with death rates roughly double those of white Americans. – NY Times
“Maybe that’s the Achilles’ heel that the virus utilizes to evade our protective immune responses — by hiding in this place,” said Dr. Vishwa Deep Dixit, a professor of comparative medicine and immunology at Yale School of Medicine.
According to Stanford’s Dr. Blish, “This could well be contributing to severe disease … We’re seeing the same inflammatory cytokines that I see in the blood of the really sick patients being produced in response to infection of those tissues.”
Mysteries of fat…
As the Times notes, body fat is more than just an inert form of energy storage. On the contrary, fat is biologically active, and produces both hormones and immune-system proteins that affect nearby cells, causing a persistent low-grade inflammation regardless of any actual infection.
Inflammation is the body’s response to an invader, and sometimes it can be so vigorous that it is more harmful than the infection that triggered it. “The more fat mass, and in particular visceral fat mass, the worse your inflammatory response,” Dr. McLaughlin said, referring to the abdominal fat that surrounds internal organs.
Fat tissue is composed mostly of fat cells, or adipocytes. It also contains pre-adipocytes, which mature into fat cells, and a variety of immune cells, including a type called adipose tissue macrophages. – NY Times
As part of the study, Dr. McLaughlin, Blish and other colleagues experimented on fat obtained from bariatric surgery to see if the tissue would become infected with COVID. They found that yes, they could – but certain immune cells known as macrophages were also susceptible, and produced a ‘robust’ inflammatory response. The team also analysed fat cells from Europeans who had died of COVID, and found the disease contained within fat near various organs.
According to Johns Hopkins professor of cardiology, Dr. David Kass, a man whose ideal weight is 170 lbs, yet who weighs 250 lbs, is carrying a substantial amount of fat in which the virus can ‘hang out’ – where it can then replicate and trigger a ‘destructive immune system response.’
“If you really are very obese, fat is the biggest single organ in your body,” said Kass, who added that COVID “can infect that tissue and actually reside there.”
“Whether it hurts it, kills it or at best, it’s a place to amplify itself — it doesn’t matter. It becomes kind of a reservoir.”
And as journalist Alex Berenson wrote in July…
In April, British researchers published a definitive paper on the subject in The Lancet Diabetes & Endocrinology, a peer-reviewed journal. The researchers examined the medical records of almost 7 million people in England to look at the link between obesity and severe outcomes from COVID, including hospitalization and death.
The top line findings show only a moderate link between extra weight and COVID risk. But when the researchers looked more closely, they found that’s because in older people, being overweight does NOT drive excess risk.
So the researchers divided the patients into four age ranges: 20-39, 40-59, 60-79, and over 80. They found that in the two younger groups – including adults up to age 60 – being obese was associated with nearly ALL the risk that COVID would lead to intensive care or death. The findings held even after they adjusted for many different potential confounding factors, like smoking, non-weight-related illnesses, and wealth.
The excess risk was extremely high even for people who weren’t morbidly obese – defined as a body-mass index of 40 or more. A person between 40 and 60 with a BMI of 35 – someone who is 230 pounds and 5’8” – had about five times the risk of dying of COVID of a person of normal weight. For younger adults, the excess risk was even higher, and for morbidly obese people even higher still.
In contrast, people of normal weight under 40 are at essentially no risk of death from COVID. The researchers found their rate to be under 1 in 10,000 per year. Even in the 40 to 59 age range, normal-weight adults had an annual risk well under 1 in 1,000.
* * *
Lose the weight, folks. And for those who need to shed pounds fast, a ketogenic diet may actually act as a preventative measure.
This article (Scientists May Have Discovered Why COVID Hits Fat People Harder) was originally published on Zero Hedge and is published under a Creative Commons license.
